The focus of this blog will be a general layout of the phases of rehab following an ACL injury. The specifics of each phase will be present in later blogs.
If you would like help with rehab following an ACL injury then please book a session here!
An ACL rupture can be a difficult injury to recover from and generally requires a long rehab to return to full function. Individuals are faced with a decision after a ruptured ACL to either opt for surgery or to go the non-surgical route. If opting for surgery then it is recommended to focus on the goals stated in the first phase of rehab before surgery and immediately after surgery. The non-surgical route will simply start with phase 1.

Phase 1: Prehab/Early Stage
The primary goals of this phase are the following:
- Reduce pain and swelling
- Increase knee range of motion (full extension & flexion)
- Increase lower limb strength
- Improve activities of daily living
- Preserve Fitness
- Manage Emotions/Stress
Reduce Pain & Swelling
Pain and swelling are common after surgery and it must be managed early. Pain and swelling can lead to arthrogenic muscle inhibition (AMI) which is a neurological reflex that weakens muscle surrounding a joint. If pain and swelling decrease then the muscles surrounding the joint will be more active. Reduced swelling will also improve range of motion into flexion and extension at the knee.
How do you manage pain and swelling at the knee?
Immediately after surgery its important to:
- Protect the injured joint initally by not performing aggravating activities and using crutches to reduce the load that the knee has to bear. Crutches can be weaned off when ready and you have spoken to your provider.
- Elevate the injured area above the heart. It can be helpful to raise the injured limb up against a wall for short periods of time.
- Icing: icing following surgery can help temporarily reduce pain and inflammation
- Light Compression: a light compression sock can be helpful to wear to reduce swelling.
- Light knee movement: this will be covered in the rest of phase 1 rehab.
Knee Range of Motion
Knee range of motion includes: knee flexion and knee extension. After surgery and also before surgery it is important to get knee extension early as this will improve the function and stability of the knee when used in daily tasks, running, walking and other strength related activities.
There are two main activities used in improving knee range of motion:
- Stretches/mobility
- Strength movements
How to improve knee extension after an ACL injury?
- Stretching into knee extension
For this we use something called a heel prop. A heel prop can be loaded or unloaded. I’d recommend using an unloaded heel prop as often as possible following injury/surgery and occasionally doing some sets with load for short periods of time. Allow the knee pain to guide how much load you use. This should not be a movement that leads to high pain and flare ups, however, there will likely be some discomfort.

- Isometrics: contracting the quads in a static position

- Isotonics: contracting the quads through a range of motion.

- Hamstring Relaxation: this can be an issue following injury or surgery particularly if there is pain going into extension. It’s important to focus on relaxing the hamstring (or relaxing the knee in general) to allow the knee to enter extension.
Leg Strength
Following any injury, its generally expected that some strength loss will occur. An ACL injury is a significant injury with a long recovery and building strength will be a primary component of rehab. This involves muscles proximal and distal to the knee. The main areas of focus for strength work should be: knee, ankle, hip. However, a full body program to develop all round fitness is optimal.
What muscles need to be strengthened at the knee joint?
- Quadriceps
- Hamstrings
- Gastrocnemius
- Adductors
What muscles need to be strengthened at the hip joint?
- Glute Maximus/Medius/Minimus
- Adductors
- Rectus Femoris
- Hamstrings
What muscles need to be strengthened at the ankle joint?
- Soleus
- Gastrocnemius
The above sections mention some of the major muscle groups, but not all the muscles.
As you can see above, many muscles are present across multiple joints and therefore can be influenced by movement or lack of movement at that joint.
Activities of Daily Living
The main activities that must be normalised after surgery mainly involve weight bearing and walking. Being able to bear your body weight supported by the knee and also being able to return to normal walking are foundational to continue with rehab. Walking normally usually comes back as the knee range of motion improves, swelling decreases, and pain improves. There are some movements that you can perform to help improve your ability to bear weight through your leg which will be addressed in another article.
Preserving Fitness
Fitness levels usually drop quite significantly after an ACL injury because it requires a significant amount of time doing less than you were likely doing previously. Not all people who have an ACL injury are highly active, however, many are. Being able to preserve as much fitness as possible during this time and improving this throughout rehab will be extremely important to knee function, general fitness & health.
During phase 1, you may want to take some brief time away from strenuous movements. Once you are able to, cycling and swimming are great ways to maintain fitness without putting much load through the knee. Cycling will require some range of motion before being able to complete full revolutions, but this can be achieved relatively soon.
Managing Stress and Emotions
Questioning why this injury happened to you, feeling helpless, believing you’ll never get back to your previous level of fitness or performance, fear, frustration, anger and anxiety are all normal thought and emotions which must be addressed with a trusted professional who encourages positivity and a clear plan to return to previous levels of performance.
Phase 2: Mid Stage - Strength & Conditioning
Each phase of rehab has some general guidelines on when to transition to the next phase. Many individuals try to rely on time alone to decide when to progress rehab but the reality is that everyone will progress at different rates.
The mid-Stage is when a lot of the usual strength and conditioning style training gets introduced as the knee is able to withstand more load than previously.
The primary goals within this phase are:
- Muscle strength and hypertrophy
- Movement Quality
- Fitness
Additionally, range of motion and swelling/pain will likely still be a factor that has to be managed or improved but in this phase its usually less of an issue.
What exercises should you be performing to improve muscle strength for ACL rehab?
The same muscles focused on in phase 1 will also be the focus in this phase, however, it will involve much more variation and other progressions.
Some movement patterns during this phase include:
- Squat Pattern
- Hinge Pattern
- Quadricep Isolation
- Hamstring Isolation
- Adductor Isolation
- Calf Isolation

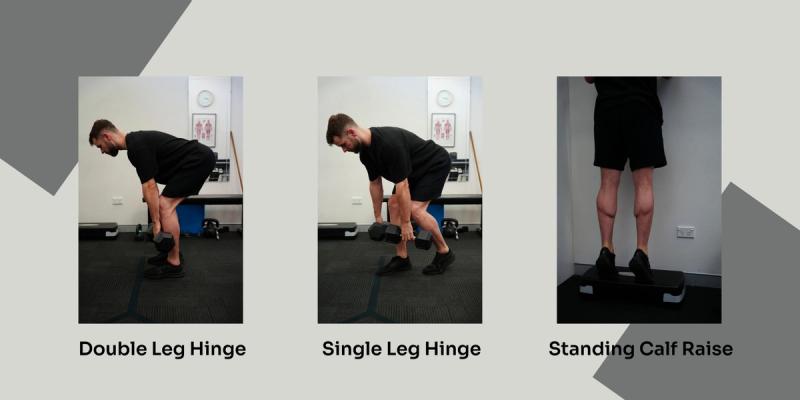
All movement patterns have double and single leg variations. They also have isotonic, isometric & eccentric variations. There are basically unlimited options for progression and its important to find movements that work for you. There is no perfect or gold standard ACL program and all programs can be changed to suit your lifestyle, preferences and capabilities.
What movement quality standards need to be considered during ACL rehab?
Following injury, the lower limb can have significant changes to balance, sense of joint position (proprioception), limb control. Many of these factors are a result of a significant lack of strength, pain, swelling and instability due to alterations to the structure of the joint.
Movement quality issues that arise following ACL surgery include: intra-limb compensations and inter-limb compensations.
Inter-limb: compensations made on the uninjured limb to account for deficits in function in the injured limb. Eg. this usually results in shifting bodyweight to the uninjured leg during squats, walking, running etc.
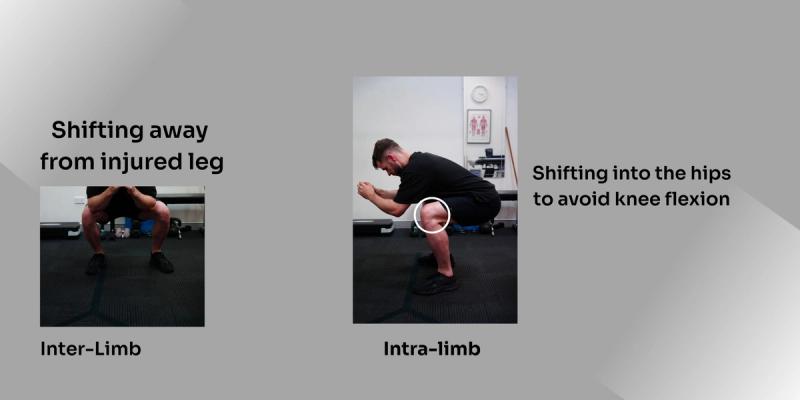
Intra-limb: compensations that occur within the injured limb. This could include avoiding knee flexion and shifting load to the hip or ankle on that side. Eg. squatting with a significant torso lean to avoid knee flexion. It could also involve sprinting where an individual tends to maintain knee extension when slowing down (trying to avoid using their quads to decelerate).
How to regain fitness during ACL rehab?
Regaining fitness to levels back to previous standards and beyond requires strength training of the lower and upper limb, conditioning that is preferably non weight bearing until running is a viable option later in rehab. Some other options for conditioning include cycling & swimming.
Phase 3: Mid-Late Stage - Running & Plyometrics
This phase primarily focuses on introducing plyometrics at a low level. True plyometric movements involve jumping, hopping & sprinting movements that have a ground contact time of less than 0.25 seconds.
Plyometrics are a great way to expose the limbs to greater forces and help prepare individuals for other plyometric activities such as running & change of direction. Plyometrics also help to build confidence in the injured limb by progressively increasing the intensity and duration of plyometrics.

Additionally, this phase includes returning to running which must be gradual to allow the injured leg to adapt to the new stimulus. Running progress could start with low intensity activity such as 50% intensity runs at 20-50 metre distances. Over time this can be progressed to greater and greater intensities and distances. By the end of this phase you will be prepared to begin higher speed running and sprint training which leads into phase 4.
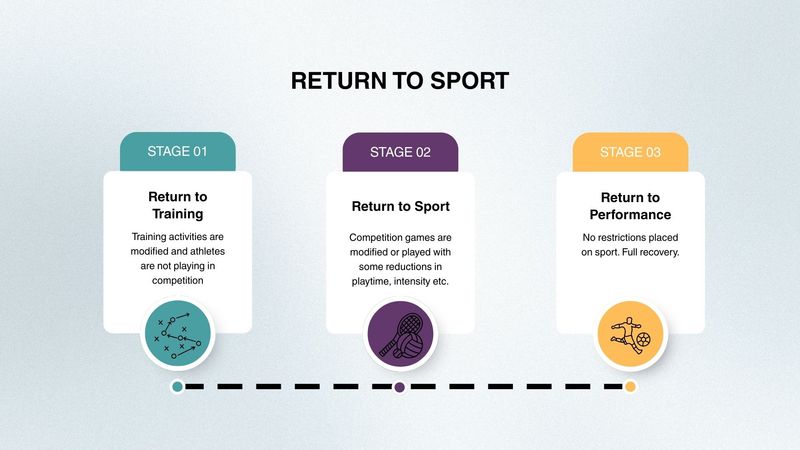
Phase 4: Late Stage - Sprinting, Change of Direction & Return to Sport
The final stage of ACL rehab involves sprinting, change of direction & deceleration training. This is then followed by a return to training, sport and eventually a return to full performance.
Sprint training will generally involve some form of deceleration activity because you must come to a stop after sprinting. The intensity of the decelerations can be manipulated by the speed of the sprints and the distance allowed to stop. Deceleration is the likely mechanism to which the ACL was initially injured and this is why it is introduced heavily in the final phase of rehab.
Return to Sport:
When returning to sport it is important to know that it will not be immediate and will initially require some time returning to light training to gain practice with some sport specific movements. This will then lead to full training sessions followed by a return to sport. Returning to sport will initially have some reductions in play time/ intensity. Following this, there is a full return to performance and this represents a full recovery.